Japan’s public health and culture, and the ongoing fight against COVID-19
Abstract
The rising number of new cases or new waves of COVID-19 infections threaten to overwhelm or collapse the health care system in many countries. The pandemic is likely to make the human sufferings worse. However, unlike many other developed countries, the situation in Japan with respect to COVID-19 remains relatively very good, despite the existence of a number of unfavorable factors that could make the country more vulnerable to COVID-19. Therefore, it seems important to understand and clarify the factors that have helped hold down the number of COVID-19 cases and deaths in Japan. The purpose of this narrative review was to provide some insights into the public health system and cultural factors that might have significantly contributed to the success of Japan in the fight against COVID-19. In light of the findings and discussion of this review, we suggest that Japan has achieved a remarkable success against COVID-19, by virtue of its strong and effective public health system, and also high standards of ingrained hygiene practices that are deeply influenced by local culture.
INTRODUCTION
During the last 20 years, we have faced six infectious epidemics―SARS and MERS, avian flu and swine flu, Ebola and Zika virus. Now we are facing the crisis of COVID-19 outbreak, the rapid spread of which has caused an unparalleled health and economic crises globally. COVID-19, the disease that is caused by the novel coronavirus (2019-nCoV), emerged in Wuhan (the epicenter of the outbreak) last December. Subsequently, WHO Director General declared it as a Public Health Emergency of International Concern (PHEIC) on 30 January 2020 [1]. COVID-19 continues to pose dramatic and serious threats to public physical and mental health and well-being. As of 3rd August 2020, there are about 18,221,215 reported confirmed cases of COVID-19 and 692,384 deaths worldwide [2], and the numbers are increasing every day. The number of new infections or the new wave of infections threatens to collapse the health care system in many countries of the world. The pandemic is also taking a catastrophic toll on the global economy and likely to make the human sufferings worse.
Japan, a country with strong trade and tourism ties with China and very close to it, was among the first countries in the world to be affected by the novel coronavirus after China [3]. Furthermore, a number of unfavorable factors made Japan a very fertile field for the potential spread of the novel coronavirus:
- Japan ranked first on the list of popular overseas destinations for Chinese tourists in 2019. In January 2020, Japan received an estimated total of 925,000 visitors from China [4]. This probably caused more exposure of Japanese people to tourists and travelers from Wuhan.
- Japan, a country with very densely populated cities, has a super-aged society with the world’s highest proportion of population aged 65 years or over. Rising burden of chronic diseases and various comorbidities associated with aging and declining immunity, pose an increased risk of getting severely ill from COVID-19 and with dramatically higher case fatalities associated with the latter [5].
- Japan has no national public health agency comparable to the Centers for Disease Control and Prevention (CDC) in USA, China and South Korea. CDC provides expert and critical decision-making advice to the government during a health crisis and also provides necessary important and urgent public guidance with the accurate and up-to-date information. Furthermore, like the National Library of Medicine in USA, a national online platform on life science and biomedical research is absent in Japan. Such databases can provide the citizens with easily obtainable up-to-date, evidence-based and accurate information in the native language. On the other hand, unlike other developed countries, the people in Japan make relatively little use of digital tools [6]. Until recently, no high-tech application was available in Japan to stem the spread of the coronavirus. Only very recently, the government of Japan launched a coronavirus contact-tracing free smartphone application [7]. Furthermore, Japan has a shortage of doctors specializing in infectious diseases. According to the National Institute of Public Health, 33% of Class 1 hospitals are lacking in infectious disease specialists [8]. Moreover, during the recent outbreak, Japan faced a dilemma initially over the lack of adequately prepared infectious disease departments and a stockpile of personal protective equipment (PPE) [9]. All these raise the question on whether Japan has the proper scientific infrastructure to respond to a viral outbreak.
- In order to monitor and control the COVID-19 pandemic, WHO made a strong recommendation to perform more tests for the potential coronavirus cases. In contrast, Japan’s testing rate for coronavirus remains the lowest among the developed countries [10]. As Japanese government’s coronavirus response was more or less sluggish with reluctance to carry out extensive testing for the new coronavirus, this was probably caused by the consideration of adverse impacts on a slow-growth economy associated with the postponement or cancellation of Tokyo 2020 Summer Olympics.
- Also, compared to other countries, Japan’s initial response was slow to block or limit arrivals of travelers from China and other regions, hit especially hard by the COVID-19 outbreaks. The Chinese President Xi Jinping’s state visit to Japan, originally planned for early April, probably also played a role in such a decision regarding the entry of those travelers to Japan.
- To curb the spread of the new coronavirus, Japan did not introduce any lock-down as a measure of social distancing, as seen in many other countries. On the other hand, the state of emergency in Japan was imposed with polite requests to the citizens – strictly voluntary and not as a legal obligation.
- In March, Japanese people could not refrain from going outside for enjoying ‘hanami’, when cherry blossoms reached full bloom. It caused the chances of interpersonal contacts and the spread of the coronavirus higher.
- The general health literacy of Japanese is lower than their European counterparts, which indicates their difficulties in acquiring and processing healthcare information and making sound health decisions [11].
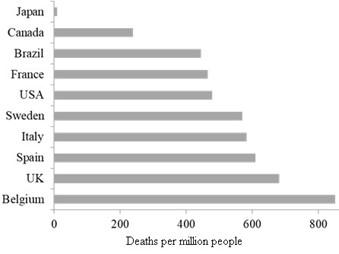
Considering all the issues and factors mentioned above, Japan was expected to have a coronavirus explosion with a high number of infections and coronavirus deaths. In contrast to the gloomy forecasts by different experts, politicians and various media, the situation in Japan with respect to the new coronavirus remains relatively very good! Japan has been able to keep the deaths from COVID-19 low compared with most of the other coronavirus-stricken countries. As we can see in the following figure, the death rates are surprisingly lower in Japan (8 deaths per 1 million population) in comparison to some of the hardest hit countries, such as Belgium (849 per million), UK (680 per million), Spain (608 per million), Italy (582 per million), Sweden (568 per million), USA (478 per million) and, France (464 per million) [12] (Figure 1). It should be noted here that a few other countries have much lower death rates than that of Japan like Thailand (0.8 per million), Sri Lanka (0.5 per million), Taiwan (0.3 per million), Vietnam (0.06 per million), and Mongolia with zero deaths from COVID-19 [12]. However, like the latter countries, Japan did not impose harsh measures like closure of borders, complete lockdowns, and large-scale testing or strict implementation of quarantines. Also, those countries do not have a rapidly ageing population like that in Japan (proportion of population aged 65 years or over: ranging between 4.2% in Mongolia to 14.9% in Taiwan versus >28% in Japan) [13, 14]. Considering such facts and other above-mentioned factors that made Japan more vulnerable to COVID-19, it is obvious that Japan has been able to keep the deaths from COVID-19 low compared with most of the other coronavirus-stricken countries. In Japan, the state of emergency has been completely lifted on May 25, 2020; life is quickly returning to normal with some precautions.
Therefore, it seems important to understand and clarify the factors that have made the prevention and mitigation of the current coronavirus outbreak possible for the Japanese people. Also, understanding Japan’s experiences in the control of the COVID-19 outbreak might provide important lessons for the global health community, especially for the countries struggling to deal with the ongoing pandemic and might help to better prepare for future epidemics or pandemics of novel infections. Currently, there is no vaccine against COVID-19 and/or proven effective or specific treatments for it. Also, there is a lack of clear understanding on the characteristics of the novel coronavirus and environmental factors influencing the virus persistence in the environment. In light of these facts, in this review, we provided some insights into the public health system and also cultural factors that might have helped Japan to hold down the number of COVID-19 cases and deaths
JAPAN’S RESPONSE TO COVID-19 AND ITS PUBLIC HEALTH
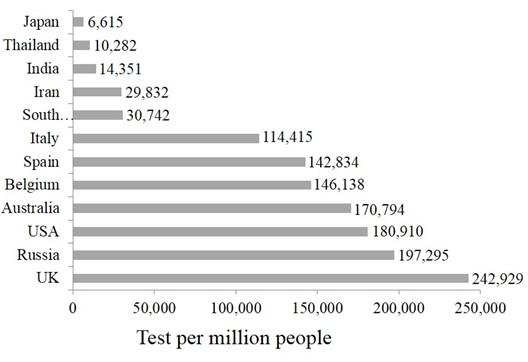
Japan did not heed to the advice of the World Health Organization (WHO) to perform mass testing to detect the coronavirus; instead, limited coronavirus tests were conducted in Japan for which the government drew widespread criticism. Over the past few months, there is a gradual increase in coronavirus testing; but Japan still lags far behind other developed countries [12] (Figure 2). However, from the public health point of view, there was an important reason for Japan’s relatively restrained approach on coronavirus testing. The existing Infectious Disease Law in Japan mandates hospitalization of each patient infected with a Category-II disease (like COVID-19), irrespective of the severity of the disease. The public health authorities worried that potential confirmation of a large number of coronavirus cases could cause the admissions of those even with mild symptoms or without symptoms, accordance to the law, which in turn would lead to the overflows of the specialized hospital wards and overwhelm the health care system. All these would make it difficult to treat the critically ill patients or those with urgent needs requiring intensive care. Therefore, Japan prioritized the public health perspective focusing on the prevention of severe cases, rather than the diagnosis and admission and treatment of each individual patient and conducted a limited number of tests for the coronavirus. Thus, overburdening of the hospitals was avoided and collapse of the health care system was prevented [15]. However, in recent days, there is an increase in testing capacities, and a modified strategy of pro-active testing has been suggested for this purpose [16]. This strategy includes suitable testing guidelines for each of the following 3 categories of people: (1) Category 1- People with symptoms (should be tested immediately); (2) Category 2 ― People without symptoms, who have been assessed with a high pre-test risk of infection, and/or who work in high-risk areas (should be tested in a more pro-active manner); (3) Category 3 ― People without symptoms, who have been assessed with a low pre-test risk of infection, and who work in low-risk areas (further consensus is necessary regarding the testing strategy for this group). Now the situation of COVID-19 is continuously being monitored and the appropriate information is constantly being updated.
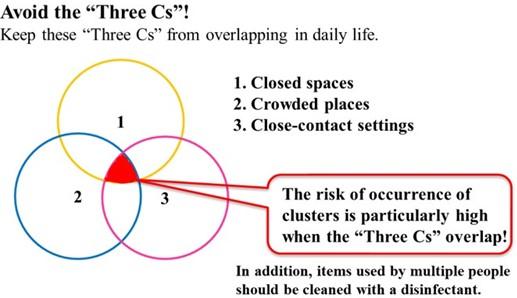
In Japan, the public health authorities introduced a special social distancing campaign ― known as “Three Cs” (closed spaces, crowded places, close-contact settings; Figure 3) ― with an easily understandable message to the public to prevent the occurrence of coronavirus clusters [17]. Also, the Japanese people have higher public health consciousness. Altogether, the “Three Cs” campaign appears to be very effective in avoiding high-risk environments by the public, instead of keeping away from each other entirely (e.g. lock-downs) [18].
At an early stage of the COVID-19 outbreak, Japanese public health experts identified the characteristic mode of transmission as human-to-human transmission clusters and suggested for prevention of formation of such clusters, which might have helped to suppress the virus transmission in Japan [19, 20]. Furthermore, this cluster-based approach uses thorough and retrospective tracing of the contacts to patients with COVID-19, which helps to suppress the further spread of the infection.
Japan has established a strong public health care system since the end of World War II. In Japan, the National Health Insurance Law was implemented in 1938, and the universal health insurance coverage was achieved in 1961 [21]. The national health insurance system provides easy access to medical care and enables anyone to receive the high-quality medical care anywhere anytime. Moreover, to identify and report any new infections to the health ministry, a nationwide network of public health centers (hokenjo in Japanese) was established by the government of Japan in 1950s [21]. This excellent system of public health centers are local government authorities and responsible for the public health of the country [22]. In 2018, the centers employed more than half of 50,000 public health nurses, who are experienced in common infectious diseases [23]. Currently, these centers are providing consultations for COVID-19. Also, they are engaged in transport of samples to the test centres and safe transport of confirmed positive cases to the designated hospitals, and contact tracing for COVID-19. For the latter purpose, contact tracing methods for tuberculosis practiced by the public health centres are being used. All these are obviously playing important roles in the fight against the ongoing pandemic.
It has been observed that older age, obesity, cardiovascular disease, diabetes, hypertension, chronic respiratory disease, cancer, etc., are associated with an increased risk of death from COVID-19 [24, 25]. A recent report by the United States Centers for Disease Control and Prevention (US CDC) revealed that hospitalizations were six times higher and deaths, 12 times higher among those with three common underlying health conditions (cardiovascular disease, diabetes, and chronic lung disease), compared with otherwise healthy individuals [26]. In Japan, the national government launched a strategy for the prevention and control of hypertension and stroke in 1969 and introduced population-wide health education for reduction of dietary salt intake [21]. Moreover, the robust public health system in Japan focuses on disease prevention strategies with improvements in healthy lifestyles (e.g. diet and nutrition, exercise, reduction in smoking and alcohol consumption) and preventing onset of life-style related diseases like hypertension, diabetes, cardiovascular disease (CVD) and cancer [27]. Moreover, a variety of public health programs are being organized in order to keep the elderly healthy and active as long as possible [28]. In Japan, the prevalence of overweight and obesity, risk factors for CVD and diabetes, are 21.4% and 4.1%, remarkably lower than the OECD averages of 34.6% and 18.0% respectively; alcohol consumption is well below the OECD average [8, 29]. Now Japan has the lowest rates of obesity, CVD mortality, and the lowest admissions for asthma and chronic obstructive pulmonary disease (COPD) in the OECD [8, 29]. It is noteworthy here that among the OECD countries, Japan has the most extensive range of health check-ups and screenings for the entire population [8]. Therefore, it can be assumed that a relatively lower prevalence of comorbidities such as hypertension, diabetes, cardiovascular diseases, lung diseases, etc., among the elderly in Japan has partly played a role in a lower death rate due to COVID-19.
Considering all the above-mentioned facts, it is reasonable to assume that a strong and effective public health system has demonstrated its strength and helped Japan in the fight COVID-19. The role of the public health system and strategies in Japan against COVID-19 has been summarized and presented schematically in figure 4.
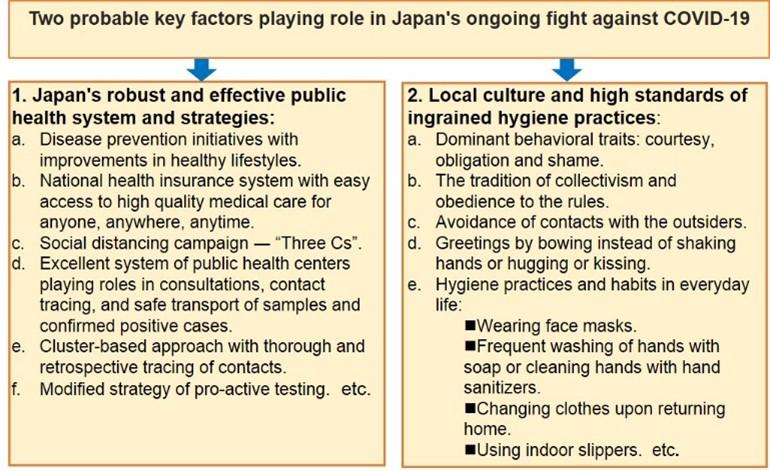
JAPANESE CULTURE AND ITS IMPACTS ON THE SPREAD OF COVID-19
In recent months, there is a lot of discussion on the possibility of regional differences in genetic susceptibility and/or immunity to COVID-19, possible past exposure to other strains of coronavirus, and the existence of some unknown so-called “Factor X” that could probably explain the mortality differences between Japan and other countries. However, these are just speculations and not proven. Rather, from the experiences of the successful countries in the fight against COVID-19, it is clear that dramatic reduction in the transmission of the virus has played the pivotal role. And here comes something special about Japan ― it’s unique culture (Figure 4)!
Responses to epidemics or pandemics seem to be closely related to local cultural values as self-care, self-sacrifice and taking care of others – all can influence individual and collective roles in the fight against an epidemic [30]. Courtesy (acting out of genuine concern for others), obligation (placing others needs before those of oneself) and shame (for not complying with group or societal norms) are three dominant motivating factors for the Japanese, which play determining roles in their cultural behaviors [31]. They also have strong moral values and higher sense of solidarity and conformity to overcome adversity [32]. On the other hand, East Asia has the history of sufferings from various infections such as malaria, leprosy, typhus, and tuberculosis. To prevent the spread of such diseases, culture-gene coevolution of collectivism of the host populations has occurred [33, 34]. Such genetic polymorphisms helped to adapt to the principle of preferring groups rather than individuals. The tradition of collectivism, in contrast to European individualism, focuses on group coordination, harmony and obedience to the rules of the group, and also avoidance of contacts with the outsiders. All these have been reflected in the fact that unlike the United States and many other countries of the world, Japan’s government did not feel the need to impose any lockdowns or fines for breaking any coronavirus rules under the state of emergency. Instead, across Japan, the public responded more or less positively to the polite request of the government to suspend nonessential businesses and stay at home as much as possible, in order to prevent the spread of COVID-19.
Hygiene practices are closely tied to Japanese culture. In Japan, there is widespread use of face masks to defend against pollen allergies and prevent transmission of seasonal influenza. Besides these, Japanese people also wear face masks as a form of social responsibility, to prevent the potential spread of infections to others. A number of recent studies have suggested that wearing face masks in public might help in mitigating the spread of COVID-19 [35-37]. According to the estimates of that study, as many as 230,000–450,000 COVID-19 cases have been possibly averted by 22 May 2020, in the United States only, due to the policy mandating public or community use of face masks. According to the expert panel of Japan government on COVID-19, mask-wearing ― anathema to many in the United States ― might be a reason why Japan has avoided the heavy coronavirus death tolls seen in many other countries in the world [38].
Japan has a widespread reputation for cleanliness in everyday life [39]. As already known, one can get COVID-19 by touching a surface or object containing the virus and then touching own mouth, nose, or possibly eyes [40]. In contrast, ingrained hygiene practices in everyday life, such as frequently washing hands with soap or cleaning hands with hand sanitizers, changing clothes upon returning home, leaving the outdoor shoes outside and using indoor slippers, proper home ventilation etc., have played important roles in fewer severe cases and fatalities of COVID-19 in Japan.
Behavioral adaptation like reduction of interpersonal contacts has been a part of human responses to infectious disease for centuries [41]. Japanese have a low-contact culture with the custom of greetings that involve bowing instead of shaking hands or hugging or kissing, and less interaction with strangers, which has also helped to minimize the spread of the novel coronavirus. Prime Minister of Japan, Shinzo Abe probably spoke of such “Japan Model” of success against the coronavirus, while announcing the lifting of the state of emergency late last May [42]. For long-term fight against the coronavirus, the government is promoting the ‘new lifestyle’ (to follow the three Cs and hygienic practices, work remotely as much as possible, exercise at home, refrain from speaking on public transportation etc.), which might help to prevent the spread of the infections while maintaining the socio-economic activities in a sustainable manner [43].
MAIN RECOMMENDATIONS
Currently, there is no proven medicine to successfully treat COVID-19 or no vaccine to prevent the infection with the virus. At this point, for the prevention or control of infectious disease threats like COVID-19: 1) a robust, efficient and effective national public health system is crucial; 2) proper risk communication by the government customized to reach the target population and cooperation between people is essential; 3) high standards of personal and public hygiene practices and habits should be integrated into our lifestyles.
CONCLUSIONS
Japan has achieved a remarkable success in the fight against COVID-19, probably by virtue of its strong and effective public health system, and also high standards of ingrained hygiene practices that are deeply influenced by local culture. In contrast, it seems reasonable to postulate that all these do not exclude the probability of resurgence of COVID-19 cases as the country lifted the state of emergency and is returning to normal with an increase in economic and social activities. However, we suggest that the experiences learned from this success in Japan in controlling COVID-19 hold important lessons for the countries continuing to struggle with the ongoing pandemic, and also for improved preparedness and responses towards the future outbreaks of unpredictable new infectious diseases, which would also be without readily available medications and/or vaccinations.
ACKNOWLEDGEMENT
None.
AUTHOR CONTRIBUTIONS
Conceptualization: MM, KM and TT; methodology: NY, RH and NH; original draft preparation: MM and KM; review and editing: NY, RH and NH; visualization: KM; supervision: TT. All authors read and approved the final version of the manuscript.
CONFLICTS OF INTEREST
The authors declare no conflict of interest.
References
- [1]World Health Organization/WHO (2020). Novel coronavirus (2019-nCoV). Situation Report – 11. Posted on 31 January 2020, available at https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200131-sitrep-11-ncov.pdf?sfvrsn=de7c0f7_4 (accessed on 20 June 2020).
- [2]Worldmeter (2020). COVID-19 coronavirus pandemic. Posted on 16 January 2020, available at https://www.worldometers.info/coronavirus/?utm_campaign=homeAdvegas1?%20 (accessed on 3 August 2020).
- [3]World Health Organization/WHO (2020). Novel Coronavirus – Japan (ex-China). Posted on 31 January 2020, available at https://www.who.int/csr/don/16-january-2020-novel-coronavirus-japan-ex-china/en/ (accessed on 20 June 2020).
- [4]Japan data (2020). Foreign Visitors to Japan Continue Downward Trend in January. Posted on 21 February 2020, available at https://www.nippon.com/en/japan-data/h00656/foreign-visitors-to-japan-continue-downward-trend-in-january.html (accessed on 24 June 2020).
- [5]Centers for Disease Control and Prevention/CDC (2020). Coronavirus Disease 2019 (COVID-19). Older Adults. Posted on 25June 2020, available at https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/older-adults.html (accessed on 5 July 2020).
- [6]Institut Montaigne (2020). Fighting the Coronavirus Pandemic, East Asian Responses – Japan: Self-Restraint, Path Dependence and the Shadow of the Olympics. Posted on 3 April 2020, available at https://www.institutmontaigne.org/en/blog/japan-self-restraint-path-dependence-and-shadow-olympics (accessed on 25 June 2020).
- [7]The Japan Times (2020). Japan’s coronavirus contact-tracing app launched amid privacy concerns. Posted on 19 June 2020, available at https://www.japantimes.co.jp/news/2020/06/19/national/japan-contact-tracing-app-launched/ (accessed on 26 June 2020).
- [8]Organization for Economic Co-operation and Development/OECD (2019). OECD Reviews of Public Health: Japan: A Healthier Tomorrow. OECD Publishing: Paris, France. https://doi.org/10.1787/9789264311602-en.
- [9]Nikkei Asian Review (2020). Japan’s coronavirus response is flawed – but it works. Posted on 14 May 2020, available at https://asia.nikkei.com/Opinion/Japan-s-coronavirus-response-is-flawed-but-it-works (accessed on 26 June 2020).
- [10]The Japan Times (2020). Will Japan’s virus testing policy be enough to flatten the curve? Posted on 16 March 2020, available at https://www.japantimes.co.jp/news/2020/03/16/national/japan-coronavirus-policy-flatten-curve/ (accessed on 27 June 2020).
- [11]Nakayama K, Osaka W, Togari T, Ishikawa H, Yonekura Y, Sekido A, et al. Comprehensive health literacy in Japan is lower than in Europe: a validated Japanese-language assessment of health literacy. BMC Public Health. 2015; 15: 505.
- [12]Worldmeter (2020). Reported Cases and Deaths by Country, Territory, or Conveyance. Posted on 8 July 2020, available at https://www.worldometers.info/coronavirus/#countries (accessed on 3 August 2020).
- [13]The World Bank (2020). Population ages 65 and above (% of total population). Available at https://data.worldbank.org/indicator/SP.POP.65UP.TO.ZS (accessed on 9 July 2020).
- [14]China Daily (2019). Taiwan’s aging population continues to rise. Posted on 9 September 2019, available at https://www.chinadaily.com.cn/a/201909/09/WS5d761e83a310cf3e3556a92f.html (accessed on 30 June 2020).
- [15]Reuters (2020). Japan defends cautious approach on coronavirus testing amid concerns. Posted on 26 February 2020, available at https://www.reuters.com/article/us-china-health-japan-tests/japan-defends-cautious-approach-on-coronavirus-testing-amid-concerns-idUSKCN20K1IM (accessed on 27 June 2020).
- [16]Ministry of Health, Labour and Welfare Health, Japan (2020). The new phase of COVID-19 response in Japan. Available at https://www.mhlw.go.jp/content/10900000/000648616.pdf (accessed on 21 July 2020).
- [17]Ministry of Health, Labour and Welfare Health, Japan (2020). “Avoid the three Cs”! Available at https://www.mhlw.go.jp/content/10900000/000615287.pdf (accessed on 27 June 2020).
- [18]Business Insider (2020). Japan avoided a lockdown by telling everyone to steer clear of the 3 C’s. Here’s what that means. Posted on 28 May 2020, available at https://www.businessinsider.com/how-japan-tackled-coronavirus-without-a-lockdown-2020-5 (accessed on 27 June 2020).
- [19]Furuse Y, Sando E, Tsuchiya N, Miyahara R, Yasuda I, Ko YK et al. Clusters of Coronavirus Disease in Communities, Japan, January-April 2020. Emerg Infect Dis. 2020;26(9). doi: 10.3201/eid2609.202272 (online ahead of print).
- [20]Ministry of Foreign Affairs, Japan (2020). Japan’s COVID-19 Response. Available at https://www.mofa.go.jp/files/100061341.pdf (accessed on 30 June 2020).
- [21]Japan International Cooperation Agency/JICA. Japan’s experiences in public health and medical systems: Towards improving public health and medical systems in developing countries. Research Group, Institute for International Cooperation (JICA): Tokyo, Japan, 2005.
- [22]Katsuda N, Hirosawa T, Reyer JA, Hamajima N. Roles of public health centers ( hokenjo) in tuberculosis control in Japan. Nagoya J Med Sci. 2015); 77: 19-28.
- [23]Bloomberg (2020). Did Japan Just Beat the Virus Without Lockdowns or Mass Testing? Posted on 23 May 2020, available at https://www.bloomberg.com/news/articles/2020-05-22/did-japan-just-beat-the-virus-without-lockdowns-or-mass-testing (accessed on 30 June 2020).
- [24]Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020; 323: 1239– doi:10.1001/jama.2020.2648.
- [25]Hu Y, Sun J, Dai Z, Deng H, Li X, Huang Q, Wu Y, Sun L, Xu Y Prevalence and severity of corona virus disease 2019 (COVID-19): A systematic review and meta-analysis. J Clin Virol. 2020; 127: 104371. doi: 10.1016/j.jcv.2020.104371.
- [26]Stokes EK, Zambrano LD, Anderson KN, Marder EP, Raz KM, El Burai Felix S, et al. Coronavirus Disease 2019 Case Surveillance — United States, January 22–May 30, 2020. MMWR Morb Mortal Wkly Rep. 2020; 69: 759-765. doi: http://dx.doi.org/10.15585/mmwr.mm6924e2.
- [27]Udagawa K, Miyoshi M, Yoshiike N. Mid-term evaluation of “Health Japan 21”: focus area for the nutrition and diet. Asia Pac J Clin Nutr. 2008; 2: 445.
- [28]Matsuda S. The health and social system for the aged in Japan. Aging Clin Exp Res. 2002; 14: 265-270. doi: 10.1007/BF03324449.
- [29]Organisation for Economic Co-operation and Development (2015). Cardiovascular Disease and Diabetes: Policies for Better Health and Quality of Care. Available at https://www.oecd.org/japan/Cardiovascular-Disease-and-Diabetes-Policies-for-Better-Health-and-Quality-of-Care-Japan.pdf (accessed on 27 June 2020).
- [30]Tangwa GB, Abayomi A, Ujewe SJ, Munung NS (2019). Socio-cultural Dimensions of Emerging Infectious Diseases in Africa: An Indigenous Response to Deadly Epidemics. Springer International Publishing, Cham, Switzerland.
- [31]The Japan Times (2018). Japan has a reputation for cleanliness — just don’t look in our closets. Posted on 25 November 2018, available at https://www.japantimes.co.jp/community/2018/11/25/our-lives/japan-reputation-cleanliness-just-dont-look-closets/ (accessed on 30 June 2020).
- [32]Japan Forward (2020). The Power of the Japanese in Avoiding a Coronavirus Explosion. Posted on 19 May 2020, available at https://japan-forward.com/speaking-out-the-power-of-the-japanese-in-avoiding-a-coronavirus-explosion/ (accessed on 30 June 2020).
- [33]Chiao JY, Blizinsky KD. Culture-gene coevolution of individualism-collectivism and the serotonin transporter gene. Proc Biol Sci. 2010; 277: 529-537. doi:10.1098/rspb.2009.1650.
- [34]Fincher CL, Thornhill R, Murray DR, Schaller M. Pathogen prevalence predicts human cross-cultural variability in individualism/collectivism. Proc Biol Sci. 2008; 275: 1279-1285. doi:10.1098/rspb.2008.0094.
- [35]Lyu W, Wehby GL. Community use of face masks and COVID-19: Evidence from a natural experiment of state mandates in the US. Health Aff (Millwood). 2020. doi: 10.1377/hlthaff.2020.00818 (e-pub ahead of print).
- [36]Leung NHL, Chu DKW, Shiu EYC, Chan KH, McDevitt JJ, Hau BJP, et al. Respiratory virus shedding in exhaled breath and efficacy of face masks. Nat Med. 2020; 26: 676-680. doi: 10.1038/s41591-020-0843-2.
- [37]Prather KA,Wang CC, Schooley RT.Reducing transmission of SARS-CoV-2. 2020; 368:1422-1424.DOI: 10.1126/science.abc6197.
- [38]The Japan Times (2020). Masks helped keep Japan’s COVID-19 death toll low, says expert panel. Posted on 28 May 2020, available at https://www.japantimes.co.jp/news/2020/05/28/national/science-health/masks-helped-fight-coronavirus/ (accessed on 30 June 2020).
- [39]British Broadcasting Corporation/BBC (2019). What Japan can teach us about cleanliness.Posted on 7 October 2019, available at http://www.bbc.com/travel/story/20191006-what-japan-can-teach-us-about-cleanliness (accessed on 30 June 2020).
- [40]Centers for Disease Control and Prevention/CDC (2020). Coronavirus Disease 2019 (COVID-19). How COVID-19 Spreads. Posted on 16 June 2020, available at https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html (accessed on 5 July 2020).
- [41]Fenichel E. Economic considerations for social distancing and behavioral based policies during an epidemic. J Health Econ. 2013; 32: 440.
- [42]British Broadcasting Corporation/BBC (2020). Coronavirus: Japan’s mysteriously low virus death rate. Posted on 4 July 2020, available at https://www.bbc.com/news/world-asia-53188847 (accessed on 8 July 2020).
- [43]Ministry of Health, Labour and Welfare Health, Japan (2020). Basic policies for novel coronavirus disease control by the Government of Japan (summary). Link: https://www.mhlw.go.jp/content/10900000/000634753.pdf (accessed on 21 July 2020).