Therapeutic potential of selective medicinal plants and their phytoconstituents in respiratory diseases: A review with an emphasis on COVID-19
Abstract
Respiratory diseases, spanning from mild illnesses like the common cold to more serious problems like pneumonia and COVID-19, pose significant challenges to global health and contribute significantly to morbidity and death. The emergence of COVID-19 has increased the need for efficient therapeutic approaches. This review article examines the potential of specific medicinal plants, namely Black Cumin, Licorice, and Echinacea, and their phytoconstituents in the management of respiratory diseases, with a specific emphasis on COVID-19. It synthesizes extant knowledge on the therapeutic efficacy of these plants, which have been used traditionally in Unani, Ayurvedic, and Chinese medicine to alleviate respiratory symptoms and boost immune functions. This review also discusses the immunomodulatory and antiviral properties of these three specific medicinal plants, as well as their function in the treatment of a number of life-threatening diseases. Incorporating insights from ethnomedicine and contemporary scientific research, this review highlights the urgency of exploring herbal medicines as complementary therapies for respiratory diseases and offers perspectives on incorporating these natural remedies into contemporary treatment paradigms, particularly in the perspective of combating COVID-19.
INTRODUCTION
Respiratory diseases encompass a spectrum of conditions, varying in severity from mild and self-limiting disorders like the common cold to more severe and potentially life-threatening conditions such as pneumonia, tuberculosis, and pulmonary hypertension. These diseases have consistently posed a persistent challenge in the realm of global health [1,2]. Annually, the respiratory disorder causes 2.2 million fatalities. As a result, the treatment for acute respiratory tract infection costs more than 20 billion dollars [3]. Moreover, the appearance of the novel coronavirus (COVID-19), caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has imposed an unparalleled strain on healthcare systems globally. First detected in Wuhan, China, in December 2019, the COVID-19 global pandemic has had a devastating impact on nearly every country across the entire world. The Chinese Centre for Disease Control and Prevention (CCDC) determined the causative agent from throat swab samples on January 7, 2020, and classified it as SARS-CoV-2 [4]. The SARS-CoV-2 genes exhibit less than 80% nucleotide identity and almost 90% nucleotide similarity with SARS-CoV genes [5]. The vital target of infection is the lower respiratory tract [6]. The predominant signs of COVID-19 encompass fever, parched cough, and fatigue. Less prevalent however nonetheless detectable symptoms of the condition include anosmia (loss of taste or smell), rhinorrhea (nasal congestion), conjunctivitis (red eyes), pharyngitis (sore throat), cephalalgia (headache), myalgia or arthralgia (muscle or joint pain), diverse forms of dermatitis (skin rash), emesis (nausea or vomiting), diarrhea, rigors (chills), or vertigo (dizziness). In addition to these mild symptoms, certain individuals have presented with severe complications such as organ failure, septic shock, severe pneumonia, dyspnea, anorexia, cognitive impairment, persistent thoracic pain or pressure, high fever (above 38°C), and acute respiratory distress syndrome (ARDS) [7]. Given the increased focus on respiratory disorders, it is imperative to prioritize research on innovative and efficacious therapeutic approaches.
The utilization of medicinal plants for disease treatment and public health maintenance is recognized across various countries and cultural contexts worldwide [1]. Previous research in the field of ethnomedicine has demonstrated that the utilization of plant-derived medicines has the potential to alleviate chest and nasal congestion, providing relief to inflamed airways and mitigating symptoms [2]. Multiple studies have documented the existence of antihistamine and antioxidant properties in herbal remedies, which are essential in alleviating respiratory ailments [8,9]. Concurrently, technological advancements have equipped us with the tools to more comprehensively understand the molecular pathways that explain the therapeutic benefits of these plant-derived treatments, enabling a seamless integration of traditional and modern approaches.
The scientists' tireless efforts resulted in the discovery of some vaccines for the COVID-19. Although helpful in managing the pandemic, current antiviral medications and vaccination efforts have limitations. Vaccine hesitancy, variable efficacy against emerging strains, and the possibility of adverse reactions motivate the search for additional interventions. In another sense, the COVID-19 pandemic increases the urgency of investigating alternative therapies [10]. Natural products and herbal medicines have a crucial role in drug discovery. Several studies indicated that natural products and their derivatives have significant antiviral activity and potential of inhibiting viral replication [11,12]. Furthermore, nutritional interventions are important to boost up the host immune system against different infections or diseases. Mortality and morbidity associated with measles, diarrhea, measles-related pneumonia, human immunodeficiency viruses (HIV), and malaria can be reduced through the use of vitamin A supplements. Vitamin C boosts up immune functions and shows the potentiality against SARS coronavirus, atypical pneumonia, and lower respiratory tract infections. In addition, individuals suffering from conditions such as diabetes, hypertension, cardiovascular disease (CVD), and cancer can develop a resistance to SARS-CoV-2 by consuming adequate amounts of vitamin D and vitamin E [13]. Zinc and pyrithione, when used together at a specific dosage, effectively suppress the replication of SARS-CoV [14].
Along with the availability of several medicines or vaccinations for COVID-19, it is crucial to discover new approaches to manage the transmission of this disease and inhibit its replication. There is solid attestation in favor of medicinal plants being utilized for fortifying body immune functions and treating different diseases in prehistoric systems of Unani, Ayurvedic, and Chinese traditional medicine. The objective of this review is twofold: first, to provide a concise overview of the existing knowledge concerning the three medicinal plants e.g., Black Cumin (Nigella sativa L.), Licorice (Glycyrrhiza glabra), and Echinacea (Echinacea spp.) and their phytoconstituents that demonstrate therapeutic potential in the treatment of respiratory disorders; and second, to investigate the relevance of these findings in the context of COVID-19. By bringing together various lines of research, this review seeks to pave the way for the effective introduction of herbal medicine into modern therapy regimens for respiratory diseases, with a particular focus on COVID-19.
METHODOLOGY
An extensive literature search was carried out through the well-recognized web databases (Web of Science, PubMed, Science Direct, Elsevier, Google Scholar, Wiley Online Library, Taylor and Francis, Springer, ACS, etc.) and different books using suitable keywords. The current review only includes articles published in English-language journals that meet the required information standards of quality. The information was structured and analyzed with Microsoft Excel (2010) software prior to being organized into tables and figures. The online botanical databases ‘The Plant List' (Royal Botanic Gardens, Kew, UK and Missouri Botanical Garden, USA) and ‘Tropicos' (Missouri Botanical Garden, USA) were used for taxonomic treatment of the documented plant species. Table 1 presents the comprehensive procedure of this approach.
Table 1. Finding information for therapeutic properties of three medicinal plants.
PHARMACOLOGICAL POTENTIALS OF MEDICINAL PLANTS IN RESPIRATORY DISORDERS
COVID-19, emerging from the SARS-CoV-2 virus, is predominantly a respiratory disease. A respiratory disease and COVID-19 share similar modes of transmission, infected organs, complications, and symptoms. Individuals diagnosed with chronic respiratory diseases (CRDs), including chronic respiratory failure (CRF), asthma, chronic obstructive pulmonary disease (COPD), interstitial lung diseases (ILDs), pulmonary hypertension, sarcoidosis, or cystic fibrosis (CF), were promptly identified as being susceptible to experiencing severe symptoms of COVID-19 [15]. Various viral respiratory diseases are widely recognized for their tendency to induce serious respiratory consequences, such as ARDS, mainly in vulnerable elderly adults and those with significant underlying health conditions (such as obesity, diabetes, or heart or respiratory failure) [16]. Based on available information and clinical expertise, people of any age who have severe underlying medical conditions like diabetes, CVD, asthma etc. might be at higher risk [17,18]. Alongside containment strategies, the regular treatment for COVID-19 consisted of symptomatic and respiratory support based on the patient's diagnosis. Severe atypical pneumonia is the main cause observed for the death in this disease. The infected patients are usually observed with symptoms of mild upper respiratory tract infection, which has similarities with the common cold attack. Prognosis refers to the predominant symptoms of COVID-19 comprised of fever (88-98%), nasal congestion, non-productive cough, exhaustion, pharyngitis, dyspnea, diarrhea, myalgia, and gastrointestinal disturbances [7,19]. Herbal treatment can be considered as a substitute for conventional medicines for more than a few reasons, including easy access and availability, minimum or no side effects, and economic. Indigenous knowledge about various kinds of medicinal plants often offers great insight into the way of drug development for an emerging disease. Moreover, an adaptive and powerful immune system is undoubtedly essential for the human body to defend against SARS-CoV-2 as well as respiratory infections [20]. The use of these plants can be helpful to prevent the onset of this disease by strengthening the body’s immune system [21]. Medicinal plants have curative potentials along with different complex chemical substances as secondary metabolites of different composition. Medicinal herbs and spices can positively be antimicrobial without being anti-life. Furthermore, these plants can be useful against viruses and fungal infections and support the ecosystem of the human body. The body’s immune system plays a great role in defending the body from autoimmune disorders, cancers, and seasonal allergies as it is one of the best defense mechanisms for a human body. Clinical trials and numerous scientific research on the use and efficacy of herbal plants and spices are on the rise now-a-days [22]. Maximizing the natural immunity of the body is crucially important as the host environment is supposed to be a governing factor for the attacking organism. Furthermore, throughout history, medicinal plants and their extracts have been used to treat a variety of respiratory and viral diseases. The first Chinese medicine (CM) oriented hospital started its function in Wuhan since February 2020 and the first recovery in Beijing came from the treatment with the IM [23]. In addition, plant-based, traditional, and home remedies can be used as a form of primary treatment. Numerous investigations have documented the inhibitory properties of extracts derived from medicinal plants and botanicals against the replication of various viruses, including SARS [24]. Additional studies have focused on investigating the antiviral properties of various plant extracts against strains of viruses that are unresponsive to traditional antiviral treatments. This led us to proactively investigate the antiviral properties of naturally occurring medicinal herbs. Based on these findings, it is reasonable to state that the use of medicinal plants, in addition to other types of drugs, should be addressed in order to combat or manage the respiratory diseases and COVID-19.
Black cumin (Nigella sativa l.)
For more than 2000 years, black cumin (Figure 1) has been used as an anti-microbial treatment as a popular and well-known medicinal food. The Prophet Muhammad (PBUH) specifically referred to black cumin as a remedy for all diseases, with the exception of death. It is also specified within the list of natural medication of 'Tibb-e-Nabavi', or "Medicine of the Prophet (Muhammad PBUH)" [25]. N. sativa has been shown to have a wide range of actions, such as diuretic, immunomodulatory, analgesic, gastroprotective, antioxidant, hepatoprotective, anti-inflammatory, and spasmolytic properties [26]. It has been suggested strongly for combating the COVID-19 based on recent computational findings and its therapeutic potentials against autophagy dysfunction, immune disturbance, CVD, viral, and bacterial infections [27].
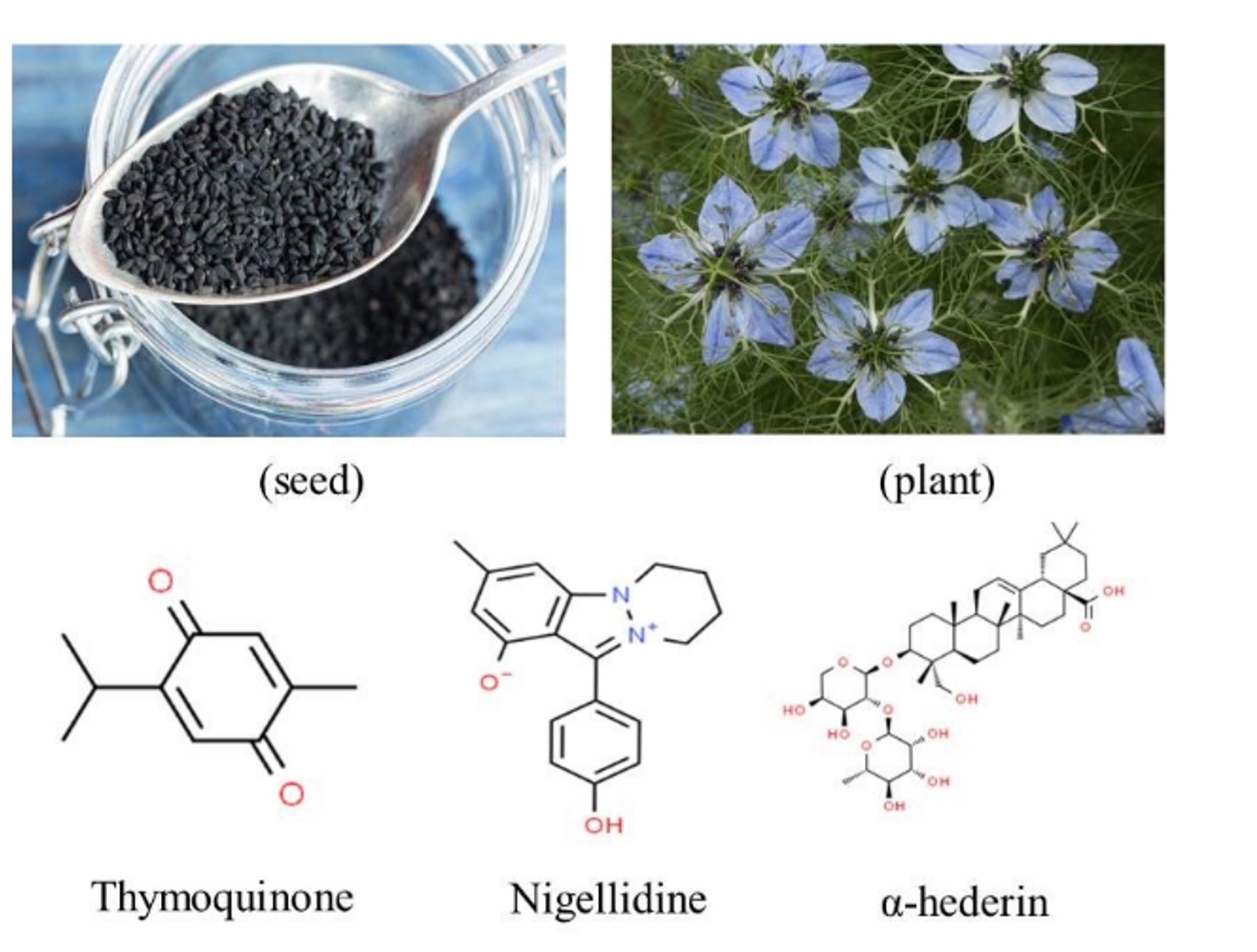
Thymoquinone
Thymoquinone (TQ) has a significant antioxidant, anti-histaminic, anti-inflammatory, anti-microbial, anticancer, and cardio-protective activities with low or no side effects [28]. TQ promotes autophagy in the human body. TQ prevents the activation of interferon regulatory factor 3 (IRF-3) by suppressing the activity of TANK-binding kinase 1 (TBK1). IRF-3 is crucial in the innate immune responses against viral and bacterial infections since it controls the generation of Type I interferons [29]. People who have rheumatoid arthritis (RA) are more susceptible to infection compared to healthy people. According to some studies, there is a possible link between RA and respiratory viral infections like parainfluenza or coronavirus [30]. Arthritis scores and pro-inflammatory cytokines levels (interleukin 1 beta,1L-1β and tumor necrosis factor alpha, TNFα) were significantly controlled by TQ, as found in a study on adjuvant-induced arthritic rats [31]. Therefore, this capability of TQ could decrease the severity of arthritis. The use of black cumin oil enhances insulin levels, reduces hyperlipidemia, promotes the growth of pancreatic islet cells, and increases the activity of hepatic antioxidant enzymes while also boosting glycogen levels [32]. Viral infections can cause apoptosis that may lead to lymphocyte depletion in the host cell. Apoptosis caused due to viruses can be inhibited by antioxidants, along with the inhibition of viral replication. Thus, a linkage can be built between antiviral and antioxidant effects. TQ performs by activating the enzymes that protect cells from destruction caused by oxidative stress. Multiple studies have demonstrated that TQ enhances mRNA expression and activates several cytoprotective antioxidant enzymes, such as catalases, superoxide dismutase, glutathione reductase, and glutathione-S-transferase [33]. The powerful antioxidant effects of this substance have been assessed using in-vivo and in-vitro experiments [34]. Severe lung injury and upper respiratory tract infection was observed in patients suffering from COVID-19. And almost all patients of COVID-19 are suffering from pneumonia [5]. A couple of in vivo studies showed the protective effects of N. sativa and its oil on lung tissue damage [35,36]. TQ is an effective inhibitor of the majority of coronaviruses, including SARS-CoV-1, and the current coronavirus strain shares approximately 80% of its nucleotide identity with SARS-CoV-1 [37]. TQ has the potential to hinder the activity of SARS CoV2 proteases, which can decrease the replication of the virus. Additionally, TQ has demonstrated significant antagonism towards ACE 2 receptors, enabling it to disrupt the virus's entry into the host cells [33].
Nigellidine, α-hederin
These two naturally occurring compounds discovered in N. sativa has the capability to operate as active agents that can hinder the activity of the coronavirus [38]. Nigellidine and α-hederin had the highest affinity for many molecular targets associated with SARS-CoV-2 and inflammation, including the primary protease (6LU7) and main peptidase (2GTB). These two compounds were more effective than hydroxychloroquine (HCQ) and favipiravir which were among the early treatment options of COVID-19 [39]. Based on a molecular docking analysis, nigellidine and α-hederin demonstrated comparable or superior inhibition of both COVID-19 and SARS viruses compared to medications administered to patients in intensive care units [40]. Figure 2 presents a visual representation of the mechanism by which numerous compounds from N. sativa exert their pharmacological effects. Moreover, the documented outcomes of N. sativa in various in-vivo and in-vitro studies are presented in Table 2.
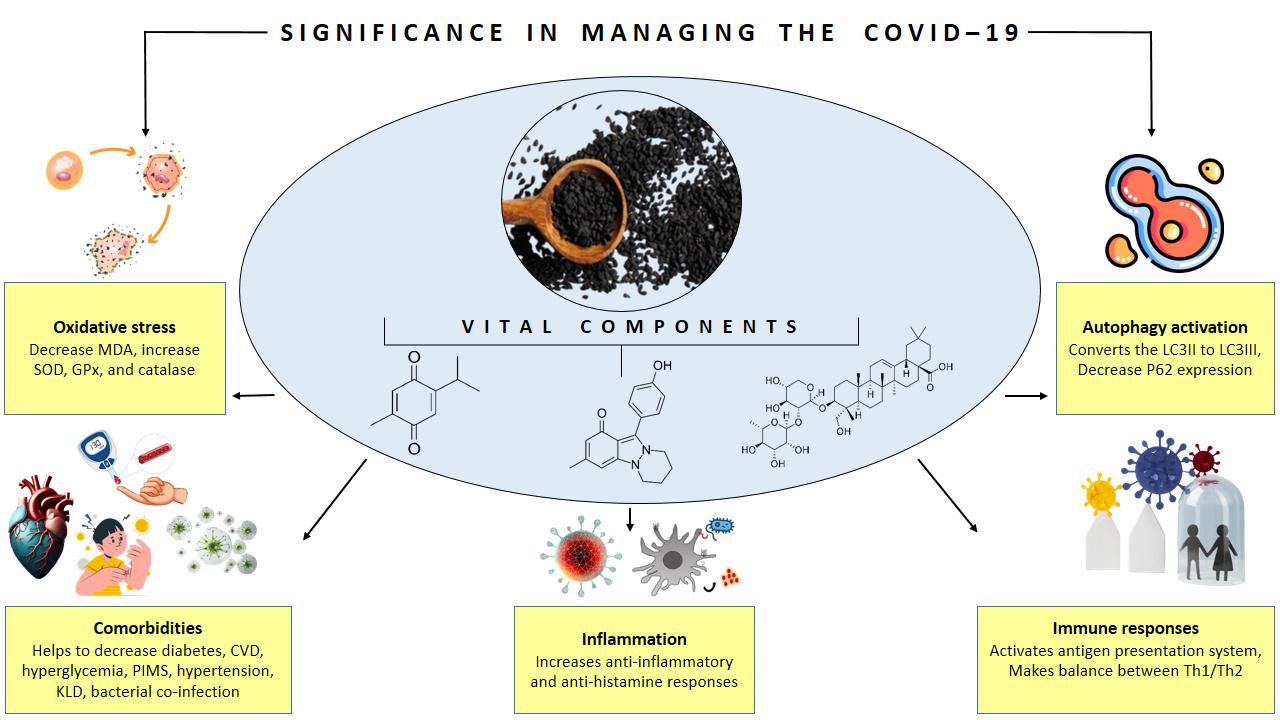
Table 2. General details and experimental studies conducted with Black cumin, Licorice, and Echinacea.
Licorice (Glycyrrhiza glabra)
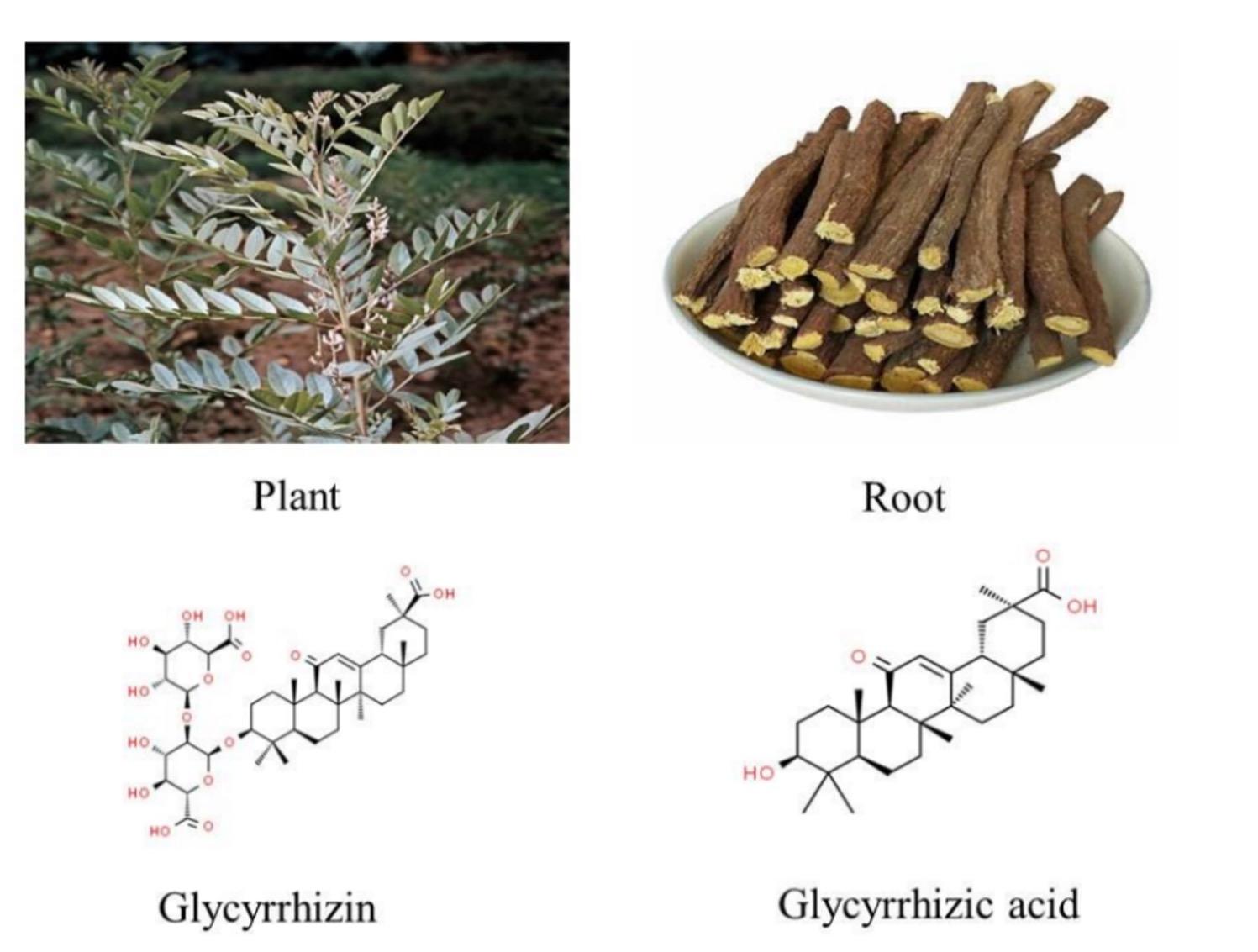
Licorice (Figure 3) has been a traditional remedy in Arabian, Chinese, Iranian, Greek, and Indian cultures for centuries [77]. Diseases like influenza, cough, liver damage, lung problems, and asthma are usually treated by licorice in oriental and folk medicine. With the ability to inhibit or slow the action of a variety of viruses, Licorice establishes itself as a broadly used antiviral containing more than 20 triterpenoids and 300 flavonoids [78]. After the emergence of COVID-19 in China, medical professionals from the State Administration of Traditional Chinese Medicine administered herbal combinations to individuals who were affected by the disease. The herbal formulation contained 6 grams of licorice which had a success rate of 90% [21,79].
Glycyrrhizin
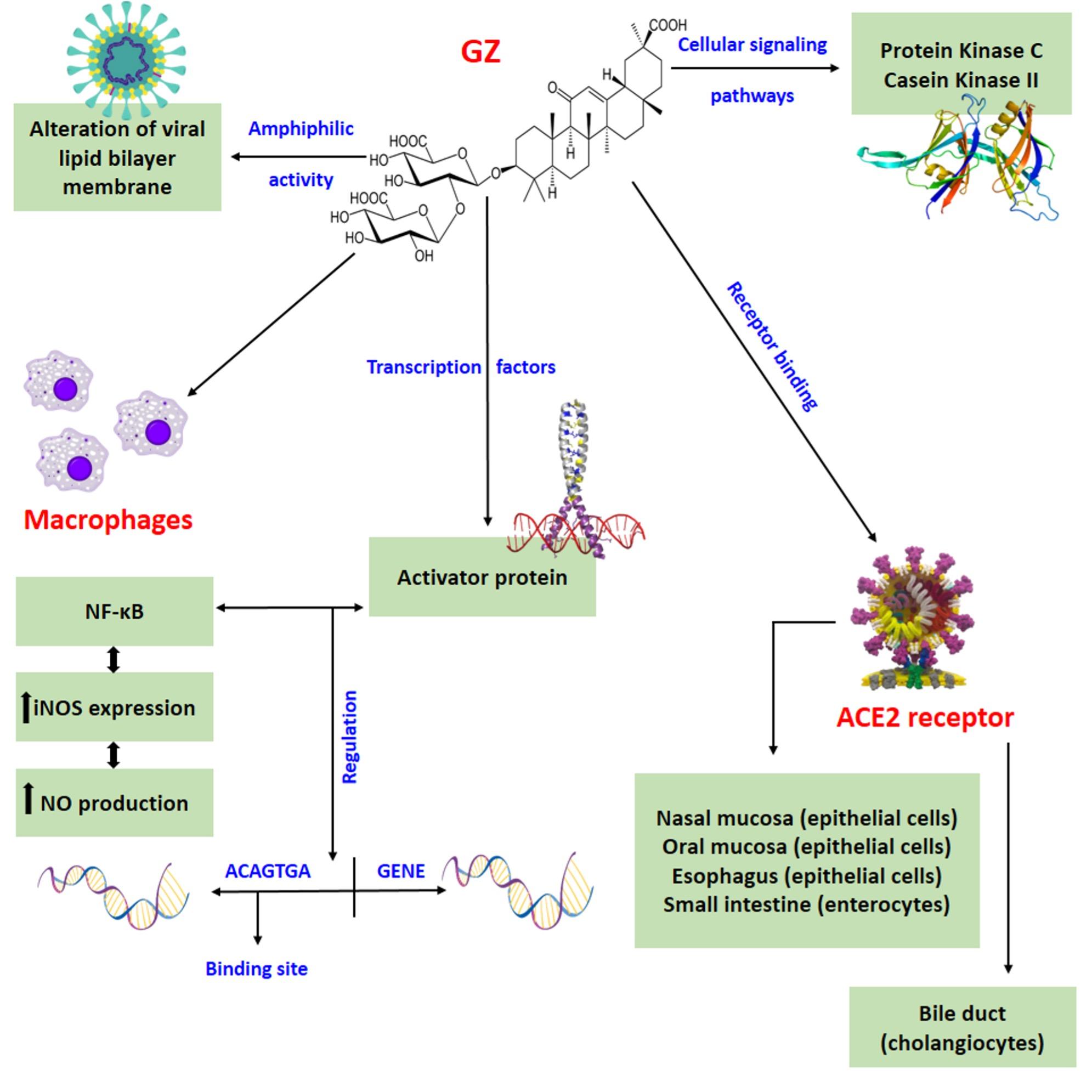
Glycyrrhizin (GZ) is usually effective against the envelope viruses like SARS related coronavirus, hepatitis D, flaviviruses, retroviruses, influenza A, herpesviruses, togaviruses, etc. as well as eleven types of flavivirus (dengue, yellow fever, Japanese encephalitis) [80]. GZ was found to be promising for the treatment of SARS [62] (Table 2). Moreover, two triterpenoids (GC and 18β-glycyrrhetinic acid, 18β-GA) of Licorice possess antiviral potential [78]. Glycyrrhizin inhibits the SARS virus in invading a target cell and reproduction of virus. Glycyrrhizin was found to be the most effective antiviral against SARS among glycyrrhizin, 6-azauridine, pyrazofurin, ribavirin, and mycophenolic acid [81]. After a molecular docking, it can be seen that glycyrrhizin possesses the potential binding to angiotensin-converting enzyme 2gene (ACE2) (estimated Gibbs free energy 9 kcal/mo; binding sites: ARG-559, GLN-388, ARG-393, ASP-30, GLN-388 and ARG-393) [82]. The researchers concluded that the binding site would be around the hydrophobic region of ACE2 based on the hydropathic nature of GZ. The infectivity of SARS-CoV-2 is greatly influenced by ACE2. Therefore, through its interaction with ACE2, GZ has the potential to inhibit the cellular entrance of SARS-CoV-2. Chrzanowski et al. [83] stated that topical use of GZ in the nasal and oral cavities could be the upper respiratory tract cells' first line of defense against SARS-CoV-2 infection. Several indicators indicate that GZ may be beneficial in treating respiratory infections and ARDS. For decades, many medicinal plant formulations containing GZ have been utilized to treat upper respiratory infections [84]. Research have proposed the utilization of GZ as a treatment for respiratory distress syndrome due to its capacity to decrease the buildup of platelets in the lungs and hinder the release of pro-inflammatory cytokines by activated inflammatory cells at the onset of the disease [85]. Figure 4 shows the action mechanisms of glycyrrhizin on SARS-CoV-2.
Glycyrrhizic acid
Glycyrrhizic acid (GA) has demonstrated efficacy in eradicating the SARS virus. GA has the ability to selectively focus on the protein structures of the SARS-CoV-2 virus and hinder its replication [86]. GA can inhibit nuclear factor-κB (NF-κB) and TNF activity which is surprisingly helpful for metabolic syndrome (MetS), ARDS, and inflammatory bowel disease (IBD). MetS is a risk factor for severe COVID-19 infection, and the recovery rate for IBS patients infected with COVID-19 is typically poor [87,88].
Echinacea (Echinacea spp.)
Echinacea (Figure 5) is considered as one of the most vital immune stimulants and used for centuries in Western herbal medicines [89]. Having the potential of increasing the number of macrophages inside the body, Echinacea has been one of the supportive herbs for the immune system with an effective antiviral, antibacterial, and antiseptic action. Usually, three species of Echinacea (E. purpurea, E. angustifolia, and E. pallid) are used to prepare various herbal preparations [89]. Echinacea medicinal formulations are commonly utilized for the prevention and management of upper respiratory tract infections [90].
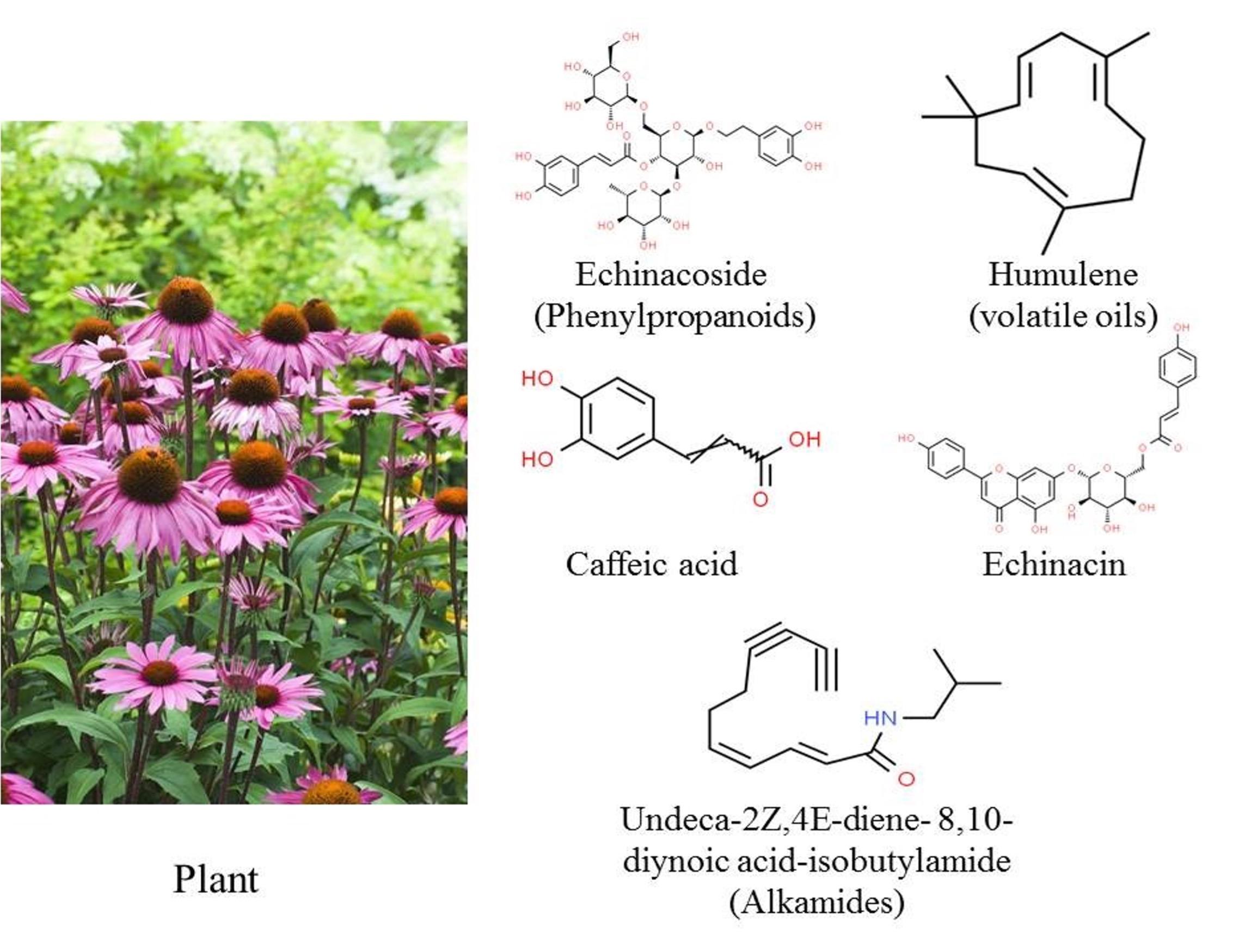
Different alkamides, phenolic, propanoids, acids, and volatile oils
Caffeic acid, chicoric acid, and echinacin are three Echinacea compounds with significant antiviral activity [72]. Viruses, like coronavirus, influenza A and B, parainfluenza, some adenoviruses, respiratory syncytial viruses, neumoviruses, as well asbocaviruses are mainly responsible for human respiratory infections [91]. Echinacea interferes with the cytokine release from these viruses and helps to relieve respiratory problems. Moreover, the polysaccharides present in Echinacea possess anti-hyaluronidase action, which inhibits the viruses from taking over the body cells [89]. Echinacea exhibits immunomodulatory properties via regulating the activity of PRRs, pathogen-associated molecular patterns (PAMPs), and DAMPs, thereby inducing an antiviral response. Upon entering the host cell, the virus triggers PAMP signals that activate innate immunity cells containing PRRs [such as TLRs, retinoic acid-inducible gene-I RIG-I-like receptors (RLRs), and nucleotide-binding proteins], hence stimulating an effective immune response against the pathogen [92]. As previously stated, increased levels of IL-6 can exacerbate the acute lung injury or even damage the organ in the COVID-19 patient. E. purpurea extracts can lower IL-6 levels and protect against lung injury. In an experimental model, E. purpurea and the alkamide dodeca-2E,4E,8Z,10Z(E)-tetraenoic acid isobutylamide restored liver enzymes, attenuated inflammation, inhibited inflammatory cytokines, and activated the c-reactive protein [93]. The presence of phenolic components and chicoric acid in Echinacea extracts is responsible for their antioxidant and free radical scavenging properties [94]. Nevertheless, the extracts contain alkamides that exhibit reduced efficacy in scavenging free radicals [94]. The redox condition of a cell directly affects its vulnerability to oxidative stress, leading to potential consequences such as cell death and the release of viruses. SARS-CoV-2 infection can disturb redox balance by affecting NAD production, poly (ADP-ribose) polymerase (PARP) function, and proteasome and mitochondrial function, resulting to enhanced cell stress responses that aggravate inflammation [92]. COVID-19 patients may experience cardiovascular, pulmonary, renal, and neurological symptoms due to inflammation and oxidative stress generated by the virus. E. purpurea has demonstrated its ability to enhance endogenous antioxidants and radical-scavenging activity through several in vitro and in vivo experiments and models, leading to a reduction in oxidative stress (Table 2). Echinacea inhibits proinflammatory cytokines as well as the Nrf2/HO-1 and NF-B/Nrf2 signaling pathways, thereby suppressing ROS generation and controlling cell proliferation and inflammation [95]. ROS production can lead to an increase in IL-6 production and lipid peroxidation, which can lead to cell damage [96]. Echinaforce, a hot beverage made from extracts of E. purpurea, has been proposed as a preventive treatment for all coronaviruses, including the recently emerged SARS-CoV-2 [97]. Figure 6 depicts how Echinacea is expected to reduce inflammatory cytokines and activate CB2/PPAR in the setting of the interplay between infection, immunity, and inflammation in COVID-19.
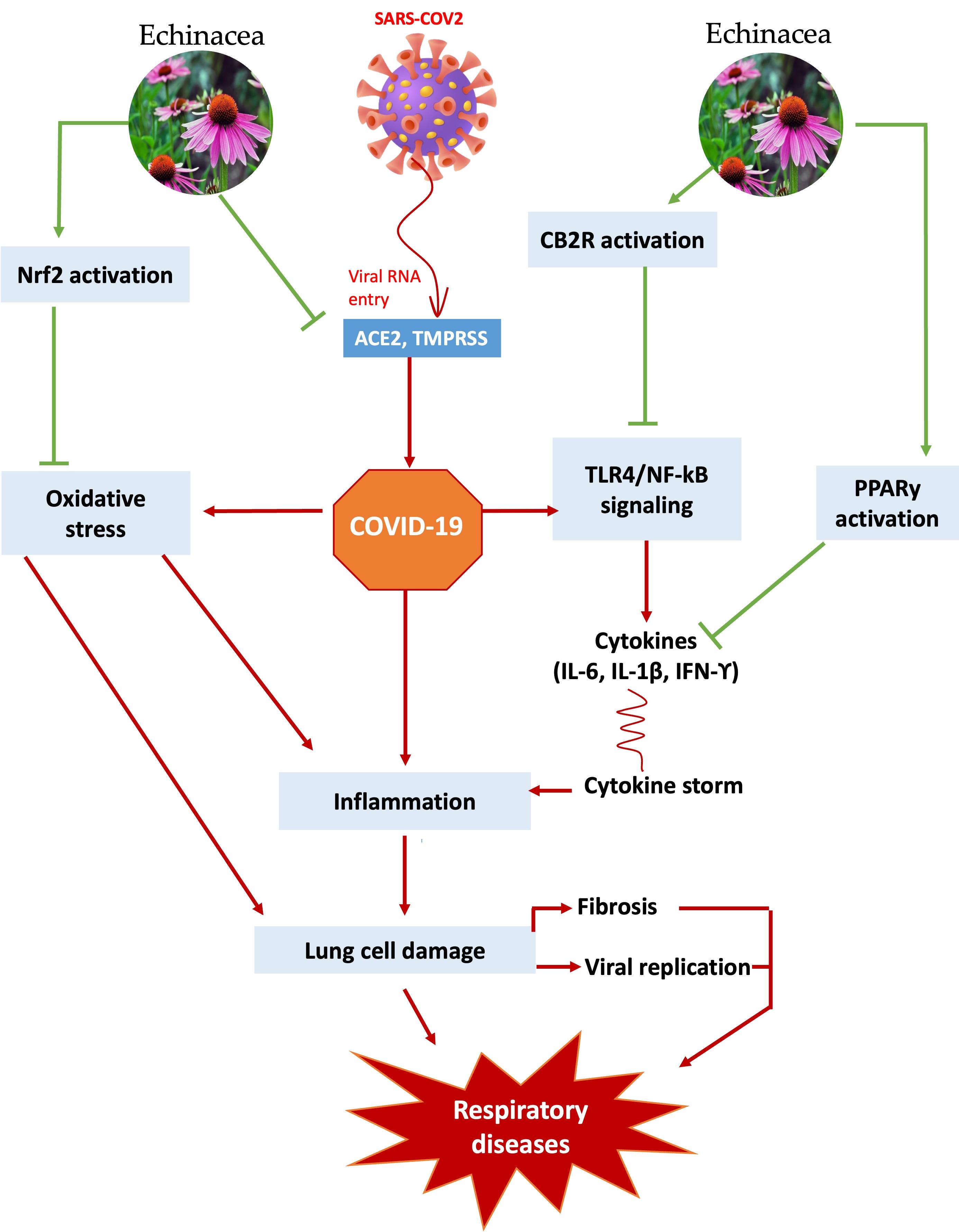
CONCLUSION AND PERSPECTIVES
Nowadays, phytotherapy provides viable options for treating respiratory infections, conditions with a high incidence in both infants and adults. The potential integration of herbal remedies into the healthcare realm in the future cannot be definitively dismissed. The utilization of this particular entity is extensive and has demonstrated effectiveness across a diverse array of contexts. Following the emergence of highly contagious SARS-CoV and middle east respiratory syndrome coronavirus (MERS-CoV), the world is now experiencing pandemic outbreak called COVID-19. This new virus belongs to the same beta-coronavirus group as its predecessors. Because of the high transmission rate and unpredictable nature to trace, the COVID-19 has posed a severe public health threat all over the world. Although some antiviral drugs are thought to be effective because of their previous efficacy in the treatment of SARS-CoV and MERS-CoV, and a number of vaccines are being developed as an emergency need, they may not be declared certain until long-term clinical trial results are available. Therefore, it is imperative to investigate potential alternatives that utilize non-traditional resources. In this review, we highlighted three potential medicinal plants which have a wide gamut of antimicrobial properties as well as pharmacological potentials, for the treatment and management of respiratory problems and COVID-19. These plants and their derivatives can play a vital role by enhancing the host immune responses and preventing virus replication, thus inhibiting further infection. Utilizing medicinal plants in lieu of conventional medications offers several benefits. Firstly, these plants exhibit fewer adverse effects when compared to synthetic drugs. Additionally, they can be cultivated domestically or found easily in natural surroundings. Moreover, there is a reduced likelihood of developing resistance to these plants as opposed to conventional antibiotics. Plants possess many bioactive chemicals that can provide a broad spectrum of medicinal benefits. Certain chemicals may not be accessible in synthetic drugs. However, adequate research and thorough clinical trials are necessary to find out accuracy in the fight against pathogenic viruses. These medicinal plants can create the new window for drug development against the COVID-19 in virtue of their natural origin, less or no side effects compared to synthetic drugs, and availability with low cost. Additionally, the current challenges will be to standardize pharmaceutical preparations and determine the pharmacokinetic properties for powdered seeds, oil, extracts, and other active constituents of these plants in order to ensure component stability. Additionally, it is crucial to consider the maximum permissible dosage and the safety of particular medical treatments for human use.
AUTHOR CONTRIBUTIONS
MFJ and MMR: conceptualization, methodology, supervision, writing – original draft; writing - reviewing and editing; MAM, MSK, TI, MB, and MSA: literature search, writing – original draft; writing - reviewing and editing; MTIL, PCD, MARM, MA, and MJU: writing - reviewing and editing, and literature search. All authors have approved the final version of the manuscript.
ACKNOWLEDGEMENT
A preprint has been published in ‘OSF preprints’ [98].
CONFLICTS OF INTEREST
There is no conflict of interest among the authors.
References
- [1]Asadbeigi M, Mohammadi T, et al. Traditional effects of medicinal plants in the treatment of respiratory diseases and disorders: an ethnobotanical study in the Urmia. Asian Pac J Trop Med. 2014;7:364-368.
- [2]Nyagumbo E, Pote W, et al. Medicinal plants used for the management of respiratory diseases in Zimbabwe: Review and perspectives potential management of COVID-19. PhysChem Earth, Parts A/B/C. 2022:103232.
- [3]Afzal S, Ahmad HI, et al. Use of medicinal plants for respiratory diseases in Bahawalpur, Pakistan. Biomed Res Int. 2021;2021.
- [4]Sohrabi C, Alsafi Z, et al. World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int J Surg. 2020;76:71-76.
- [5]Wu F, Zhao S, et al. A new coronavirus associated with human respiratory disease in China. Nature. 2020;579(7798):265-269.
- [6]Zhou P, Yang XL, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579(7798):270-273.
- [7]Chen N, Zhou M, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. The Lancet. 2020;395(10223):507-513.
- [8]Taur DJ, Patil RY. Some medicinal plants with antiasthmatic potential: a current status. Asian Pac J Trop Biomed. 2011;1(5):413-418.
- [9]Ninave PB, Patil SD. Pharmacological screening of Acalyphaindica L.: Possible role in the treatment of asthma. J Ethnopharmacol. 2022;290:115093.
- [10]Peng F, Tu L, et al. Management and treatment of COVID-19: the Chinese experience. Can J Cardiol. 2020;36(6):915-930.
- [11]Newman DJ, Cragg GM. Natural products as sources of new drugs over the last 25 years. J Nat Prod. 2017;70(3):461-477.
- [12]Lin LT, Hsu WC, et al. Antiviral natural products and herbal medicines. J Tradit Complement Med. 2014;4(1):24-35.
- [13]Liang W, Guan W, et al. Cancer patients in SARS-CoV-2 infection: a nationwide analysis in China. Lancet Oncol. 2020;21(3):335-337.
- [14]TeVelthuis AJ, van den Worm SH, et al. Zn2+ inhibits coronavirus and arterivirus RNA polymerase activity in vitro and zinc ionophores block the replication of these viruses in cell culture. PLoSPathog2010;6(11):e1001176.
- [15]Ahrenfeldt LJ, Nielsen CR, et al. Burden and prevalence of risk factors for severe COVID-19 in the ageing European population–a SHARE-based analysis. J Public Health. 2022; 30:2081-2090.
- [16]Beltramo G, Cottenet J, et al. Chronic respiratory diseases are predictors of severe outcome in COVID-19 hospitalised patients: a nationwide study. EurRespir J. 2021;58(6):2004474.
- [17]Zhou F, Yu T, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. The Lancet.2020;395(10229):1054-1062.
- [18]Wu C, Chen X, et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med.2020;180(7):934-943.
- [19]Zhang JJ, Dong X, et al. Clinical characteristics of 140 patients infected with SARS-CoV-2 in Wuhan, China. Allergy. 2020;75(7):1730-1741.
- [20]Li G, Fan Y, et al. Coronavirus infections and immune responses. J Med Virol. 2020;92(4):424-432.
- [21]Fan Y, Zhang Y, et al. Food as medicine: a possible preventive measure against coronavirus disease (COVID‐19). Phytother Res. 2020;34(12):3124-3136.
- [22]Yang QX, Zhao TH, et al. New thinking in the treatment of 2019 novel coronavirus pneumonia. Complement TherClinPract 2020;39:101131.
- [23]NATCM. Beijing’s first confirmed case of new coronavirus pneumonia cured by symptomatic and Chinese medicine treatment. National Administration of Traditional Chinese Medicine, Beijing. 2020.
- [24]Kotwal GJ, Kaczmarek JN, et al. Anti-HIV, anti-poxvirus, and anti-sars activity of a nontoxic, acidic plant extract from the Trifollium species secomet-v/antivac suggests that it contains a novel broad spectrum antiviral. Ann N Y Acad Sci. 2005;1056(1):293-302.
- [25]Ahmad A, Husain A, et al. A review on therapeutic potential of Nigella sativa: A miracle herb. Asian Pac J Trop Biomed. 2013;3(5):337-352.
- [26]Al Dhaheri Y, Wali AF, et al. Nigella sativa, a cure for every disease: Phytochemistry, biological activities, and clinical trials. In: Black Seeds (Nigella Sativa). Elsevier, 2022, pp. 63-90.
- [27]Islam MN, Hossain KS, et al. Revisiting pharmacological potentials of Nigella sativa seed: A promising option for COVID‐19 prevention and cure. Phytother Res.2021;35(3):1329-1344.
- [28]Woo CC, Kumar AP, et al. Thymoquinone: potential cure for inflammatory disorders and cancer. BiochemPharmacol. 2012;83(4):443-451.
- [29]Xiao J, Ke ZP, et al. The cardioprotective effect of thymoquinone on ischemia‐reperfusion injury in isolated rat heart via regulation of apoptosis and autophagy. J Cell Biochem. 2018;119(9):7212-7217.
- [30]Joo YB, Lim YH, et al. Respiratory viral infections and the risk of rheumatoid arthritis. Arthritis Res Ther. 2019; 21:199.
- [31]Vaillancourt F, Silva P, et al. Elucidation of molecular mechanisms underlying the protective effects of thymoquinone against rheumatoid arthritis. J Cell Biochem. 2011;112(1):107-117.
- [32]Abdelrazek H, Kilany OE, et al. Black seed thymoquinone improved insulin secretion, hepatic glycogen storage, and oxidative stress in streptozotocin-induced diabetic male wistar rats. Oxid Med Cell Longev 2018;8104165.
- [33]Badary OA, Hamza MS, et al. Thymoquinone: A promising natural compound with potential benefits for COVID-19 prevention and cure. Drug Des DevelTher. 2021;15:1819-1833.
- [34]Yimer EM, Tuem KB, et al. Nigella sativa L. (black cumin): a promising natural remedy for wide range of illnesses. Evid Based Complement Alternat Med 2019;1528635.
- [35]Tayman C, Cekmez F, et al. Protective effects of Nigella sativa oil in hyperoxia-induced lung injury. Arch Bronconeumol. 2013;49(1):15-21.
- [36]Kanter M. Effects of Nigella sativa seed extract on ameliorating lung tissue damage in rats after experimental pulmonary aspirations. ActaHistochem. 2009;111(5):393-403.
- [37]Devaux CA, Rolain JM, et al. New insights on the antiviral effects of chloroquine against coronavirus: what to expect for COVID-19?. Int J Antimicrob Agents2020;55(5):105938.
- [38]Koshak AE, and Koshak EA. Nigella sativa as a potential phytotherapy for covid-19: A mini-review of in-silico studies. CurrTher Res 2020;93:100602.
- [39]Ulasli M, Gurses SA, et al. The effects of Nigella sativa (Ns), Anthemishyalina (Ah) and Citrus sinensis (Cs) extracts on the replication of coronavirus and the expression of TRP genes family. MolBiol Rep. 2014;41:1703-1711.
- [40]Bouchentouf S,Missoum N. Identification of Compounds from Nigella Sativa as New Potential Inhibitors of 2019 Novel Coronasvirus (COVID-19): Molecular Docking Study. Preprint from ChemRxiv.2020.
- [41]Khan AU, Tipu MY, et al. In-vivo antiviral effect of Nigella sativa extract against Newcastle Disease Virus in experimentally infected chicken embryonatedeggs. Pak Vet J. 2018;38(4):434-437.
- [42]Umar S, Munir MT, et al. Protective and antiviral activities of Nigella sativa against avian influenza (H9N2) in turkeys. J. Saudi Soc. agric. Sci. 2016;16.
- [43]Hadi S, Mirmiran P, et al. Effect of Nigella sativa oil extract on inflammatory cytokine response and oxidative stress among people with type 2 diabetes mellitus: a randomized, double-blind, placebo controlled trial. ProgNutr. 2018;20:127-133.
- [44]Barakat EMF, El Wakeel LM, et al. Effects of Nigella sativa on outcome of hepatitis C in Egypt. World J Gastoentrol. 2013;19(16):2529-2536.
- [45]Lebda FM, Bamosa AO, et al. Effect of Nigella sativa on hemodynamics, hemoglobin, and blood coagulation in patients with type 2 diabetes. Egypt J Haematol. 2012;37(2):73-80.
- [46]Nikakhlagh S, Rahim F, et al. Herbal treatment of allergic rhinitis: the use of Nigella sativa. Am J Otolaryngol. 2011;32(5):402-407.
- [47]Salem AM, Bamosa AO, et al. Effect of Nigella sativa supplementation on lung function and inflammatory mediators in partly controlled asthma: a randomized controlled trial. Ann Saudi Med. 2017;37(1):64-71.
- [48]Okeola VO, Adaramoye OA, et al. Antimalarial and antioxidant activities of methanolic extract of Nigella sativa seeds (black cumin) in mice infected with Plasmodium yoellinigeriensis. Parasitol Res. 2011;108(6):1507-1512.
- [49]Salama RH. Hypoglycemic effect of lipoic acid, carnitine and Nigella sativa in diabetic rat model. Int J Health Sci. 2011;5(2):126-134.
- [50]Boskabady MH, Mohsenpoor N, et al. Antiasthmatic effect of Nigella sativa in airways of asthmatic patients. Phytomedicine. 2010;17(10):707-713.
- [51]Bamosa AO, Kaatabi H, et al. Effect of Nigella sativa seeds on the glycemic control of patients with type 2 diabetes mellitus. Indian J PhysiolPharmacol. 2010;54(4);344-354.
- [52]Salem ML, Hossain MS. Protective effect of black seed oil from Nigella sativa against murine cytomegalovirus infection. Int J Immunopharmacol. 2000;22(9):729-740.
- [53]Boskabady MH, Javan H, Sajady M, Rakhshandeh H. The possible prophylactic effect of Nigella sativa seed extract in asthmatic patients. FundamClinPharmacol. 2007;21(5):559-66.
- [54]Matsumoto Y, Matsuura T, et al. Antiviral activity of glycyrrhizin against hepatitis C virus in vitro. PloSOne 2013;8(7):e68992.
- [55]Moisy D, Avilov SV, et al. HMGB1 protein binds to influenza virus nucleoprotein and promotes viral replication. J Virol. 2012;86(17):9122-9133.
- [56]Mousa HAL. Prevention and treatment of influenza, influenza-like illness, and common cold by herbal, complementary, and natural therapies. J Evid Based Complementary Altern Med 2017;22(1):166-174.
- [57]Sasaki H, Takei M, et al. Effect of glycyrrhizin, an active component of licorice roots, on HIV replication in cultures of peripheral blood mononuclear cells from HIV-seropositive patients. Pathobiology. 2002;70(4):229-236.
- [58]Michaelis M, Geiler J, et al. Glycyrrhizin inhibits highly pathogenic H5N1 influenza A virus-induced pro-inflammatory cytokine and chemokine expression in human macrophages. Med MicrobiolImmunol. 2010;199(4):291-297.
- [59]Hardy ME, Hendricks JM, et al. 18 β-glycyrrhetinicacid inhibits rotavirus replication in culture. VirolJ. 2012;9(1):1-7.
- [60]Soufy H, Yassein S, et al. Antiviral and immune stimulant activities of glycyrrhizin against duck hepatitis virus. Afr J Tradit Complement Altern Med. 2012;9(3):389-395.
- [61]Sen S, Roy M, et al. Ameliorative effects of glycyrrhizin on streptozotocininduced diabetes in rats. J Pharm Pharmacol. 2011;63(2):287-296.
- [62]Hoever G, Baltina L, et al. Antiviral activity of glycyrrhizic acid derivatives against SARS− Coronavirus. J Med Chem. 2005;48(4):1256-1259.
- [63]Duan E, Wang D, et al. Suppression of porcine reproductive and respiratory syndrome virus proliferation by glycyrrhizin. Antiviral Res. 2015;120:122-125.
- [64]Crance JM, Scaramozzino N, et al. Interferon, ribavirin, 6-azauridine and glycyrrhizin: antiviral compounds active against pathogenic flaviviruses. Antiviral Res. 2003;58(1):73-79.
- [65]Fukuchi K, Okudaira N, et al. Antiviral and antitumor activity of licorice root extracts. In Vivo. 2016;30(6):777-785.
- [66]Alfajaro MM, Kim HJ, et al. Anti-rotaviral effects of Glycyrrhizauralensis extract in piglets with rotavirus diarrhea. Virol J2012;9(1):310.
- [67]Chen F, Chan KH, et al. In vitro susceptibility of 10 clinical isolates of SARS coronavirus to selected antiviral compounds. J ClinVirol.2004;31(1):69-75.
- [68]Rauš K, Pleschka S, et al. Effect of an Echinacea-based hot drink versus oseltamivir in influenza treatment: a randomized, double-blind, double-dummy, multicenter, noninferiority clinical trial. CurrTher Res. 2015;77:66-72.
- [69]Jawad M, Schoop R, et al. Safety and efficacy profile of Echinacea purpurea to prevent common cold episodes: a randomized, double-blind, placebo-controlled trial. J Evid Based Complementary Altern Med 2012;2012:841315.
- [70]PleschkaS, Stein M, et al. Anti-viral properties and mode of action of standardized Echinacea purpurea extract against highly pathogenic avian influenza virus (H5N1, H7N7) and swine-origin H1N1 (S-OIV). Virol J 2009;6:197.
- [71]Rininger JA, Kickner S, et al. Immunopharmacological activity of Echinacea preparations following simulated digestion on murine macrophages and human peripheral blood mononuclear cells. J Leukoc Biol. 2000;68(4):503-510.
- [72]Binns SE, Hudson J, et al. Antiviral activity of characterized extracts from Echinacea spp. (Heliantheae: Asteraceae) against herpes simplex virus (HSV-I). Planta Med. 2002;68(09):780-783.
- [73]Currier NL,Miller SC. Echinacea purpurea and melatonin augment natural-killer cells in leukemic mice and prolong life span. J Altern Complement Med. 2001;7(3):241-251.
- [74]Abdelmonem M, Kassem SH, et al. Avemar and Echinacea extracts enhance mobilization and homing of CD34+ stem cells in rats with acute myocardial infarction. Stem Cell Res Ther 2015;6(1):172.
- [75]Dogan Z, Ergul B, et al. The antioxidant effect of Echinacea angustifolia and Echinacea purpurea in rat colitis model induced by acetic acid. BratislLekListy.2014;115(7):411-415.
- [76]Sumer J, Keckeis K, et al. Novel Echinacea formulations for the treatment of acute respiratory tract infections in adults—A randomized blinded controlled trial. Front Med 2023;10:948787.
- [77]Bahmani M, Rafieian-Kopaei M, et al. A review of the health effects and uses of drugs of plant licorice (Glycyrrhizaglabra L.) in Iran. Asian Pac J Trop Dis. 2014;4:847-849.
- [78]Yang R, Wang LQ, et al. The pharmacological activities of licorice. Planta Med. 2015;81(18):1654-1669.
- [79]Yang Y, Islam MS, et al. Traditional Chinese medicine in the treatment of patients infected with 2019-new coronavirus (SARS-CoV-2): a review and perspective. Int J Biol Sci. 2020;16(10):1708-1717.
- [80]Buhner SH. Herbal antivirals: natural remedies for emerging & resistant viral infections. Storey Publishing: North Adams, MA, USA, 2013.
- [81]Cinatl J, Morgenstern B, et al. Glycyrrhizin, an active component of liquorice roots, and replication of SARS-associated coronavirus. The Lancet. 2003;361(9374):2045-2046.
- [82]Chen H, Du Q. Potential natural compounds for preventing SARS-CoV-2 (2019-nCoV) infection. Preprints. 2020;2020010358.
- [83]Chrzanowski J, Chrzanowska A, et al. Glycyrrhizin: An old weapon against a novel coronavirus. Phytother Res.2021;35(2):629-636.
- [84]Bailly C, Vergoten G. Glycyrrhizin: An alternative drug for the treatment of COVID-19 infection and the associated respiratory syndrome?.Pharm Ther 2020;214:107618.
- [85]Am Lee S, Lee SH, et al. Effects of glycyrrhizin on lipopolysaccharide-induced acute lung injury in a mouse model. J Thorac Dis. 2019;11(4):1287-1302.
- [86]Sun Z, He G, Huang N, et al. Glycyrrhizic acid: a natural plant ingredient as a drug candidate to treat COVID-19. Front Pharmacol 2021;12:707205.
- [87]Felsenstein S, Herbert JA, et al. COVID-19: Immunology and treatment options. ClinImmunol 2020;215:108448.
- [88]Tursi A, Vetrone LM, et al. Anti-TNF-α agents in inflammatory bowel disease and course of COVID-19. Inflamm Bowel Dis 2020;26(7):e73.
- [89]Hudson J, Vimalanathan S. Echinacea - A source of potent antivirals for respiratory virus infections. Pharmaceuticals. 2011;4(7):1019-1031.
- [90]David S, Cunningham R. Echinacea for the prevention and treatment of upper respiratory tract infections: A systematic review and meta-analysis. Complement Ther Med. 2019;44:18-26.
- [91]See H, Wark P. Innate immune response to viral infection of the lungs. PaediatrRespir Rev. 2008;9(4):243-250.
- [92]Meeran MN, Javed H, et al. Can Echinacea be a potential candidate to target immunity, inflammation, and infection-The trinity of coronavirus disease 2019.Heliyon2021;7(2):e05990.
- [93]Hou CC, Huang CC, et al. Echinacea alkamides prevent lipopolysaccharide/D-galactosamine-induced acute hepatic injury through JNK pathway-mediated HO-1 expression. J Agric Food Chem.2011;59(22):11966-11974.
- [94]Thygesen L, Thulin J, et al. Antioxidant activity of cichoric acid and alkamides from Echinacea purpurea, alone and in combination. Food Chem. 2007;101:74-81.
- [95]Li H, Wang D, et al. β-Caryophyllene inhibits high glucose-induced oxidative stress, inflammation and extracellular matrix accumulation in mesangial cells. IntImmunopharmacol2020;84:106556.
- [96]Nasi A, McArdle S, et al. Reactive oxygen species as an initiator of toxic innate immune responses in retort to SARS-CoV-2 in an ageing population, consider N-acetylcysteine as early therapeutic intervention. Toxicol Rep. 2020;7:768-771.
- [97]Signer J, Jonsdottir HR, et al. In vitro antiviral activity of Echinaforce, an Echinacea purpurea preparation, against common cold coronavirus 229E and highly pathogenic MERS-CoV and SARS-CoV. Virol J 2020; 17:136.
- [98]Jubayer MF, Kayshar MS, et al. A review on five medicinal plants considering the therapeutic potentials in the management of COVID-19. OSF preprints.